What is pericarditis?
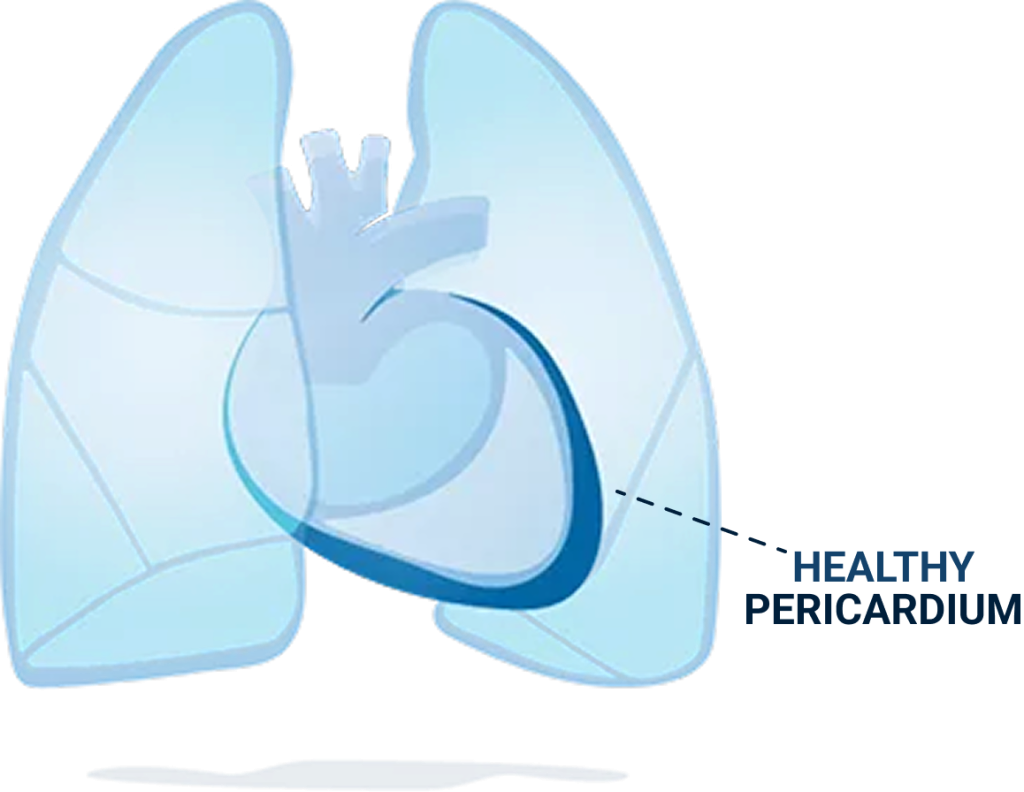
The pericardium is a thin membrane that surrounds the heart like a sac. It provides lubrication for the heart, contains it within the chest cavity, and shields it from infection and other types of harm.
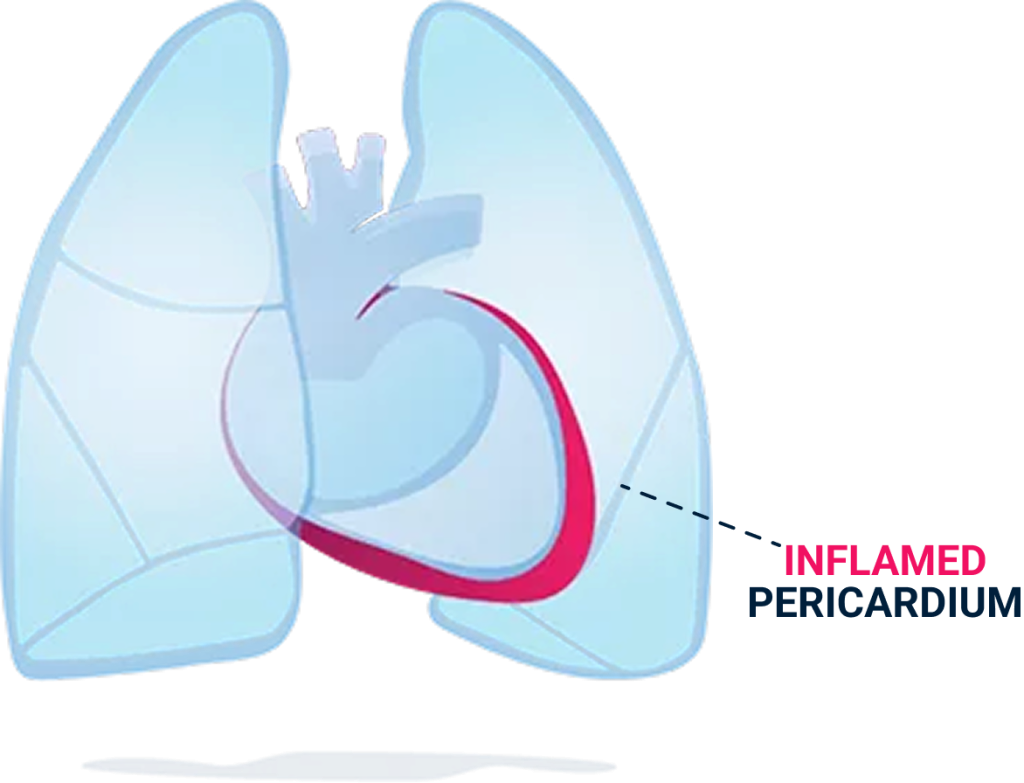
Pericarditis is a condition in which that membrane becomes inflamed (in medicine “itis” means “inflamed”). When this happens, the irritated layers of the pericardium rub against each other and can cause a lot of pain.
An episode of pericarditis is often called a flare.


Different types of pericarditis
Two types of pericarditis may include a first or one-time episode or recurrent pericarditis.
First or One-time episode pericarditis
The first episode of pericarditis is often a single flare that goes away completely on its own or after treatment.
Average duration: 4 to 6 weeks
Recurrent pericarditis
Just like it sounds, recurrent pericarditis is when a pericarditis flare happens again after a symptom-free interval of ≥4 to 6 weeks. Flares of recurrent pericarditis can happen repeatedly.
Average disease duration: often a chronic disease, with duration ~3 years for patients with 2 or more recurrences
Symptoms of pericarditis
Recurrent pericarditis may share similar symptoms with a first or one-time episode of pericarditis, but recurrent pericarditis may need to be treated differently.
Main symptom:
Chest pain, which may be so severe that it can be mistaken for a heart attack. The pain may get worse when breathing in or lying down. The pain tends to get better when sitting up and leaning forward.
Others include:


THE IMPACT OF RECURRENT PERICARDITIS

Approximately
40,000
people in the United States seek care for recurrent pericarditis annually.*
*Klein A, et al. JAHA 2021. Data from the PharMetrics Plus database, collected between January 1, 2013, and March 31, 2018, were used for this retrospective analysis (N=7502 patients with pericarditis, 2096 of whom experienced ≥1 recurrence).
With each recurrent pericarditis flare, the risk of having another flare increases.
In a study of 7502 patients with pericarditis:

of people with 1 flare had a second flare
(2096 of 7502 patients)

of people with 2 flares had a third flare
(994 of 2096 patients)

of people with 3 flares had a fourth flare
(541 of 994 patients)
With each recurrent pericarditis flare, the time in between flares decreases.
- Among patients who experienced at least 1 recurrence of a flare, the average time to flare was about 21 weeks; the average time to flare decreased by about a week for those with at least 2 recurrences of a flares, and about 3 weeks for those with at least 3 recurrences of a flare.
- Patients who had 6 or more recurrences of a flare experienced, on average, less than 12 weeks between flares.
RECURRENT PERICARDITIS CAN BE UNPREDICTABLE AND LAST FOR MANY YEARS
In a study of people with recurrent pericarditis, researchers found that the disease could last (on average) about:
6 MONTHS
for people who experienced just 1 recurrence
3 YEARS
for people who experienced 2 or more recurrences
In this study of 944 people with recurrent pericarditis (observed over 10 years), 569 had 1 recurrence and 375 had 2 or more recurrences.
CAUSES
Possible causes of a first or one-time episode
Even though a first or one-time episode and recurrent pericarditis share the same symptoms, they have different causes. For this reason, treatments that relieve symptoms in people with a first episode may not be able to prevent future flares in people with recurrent pericarditis.
There are a number of possible causes for a first or one-time episode:
*Likely caused by an undiagnosed virus or the body’s immune response to a past viral illness.
The cause of recurrent pericarditis
Recurrent pericarditis is an autoinflammatory disease, which means flares are caused by the body’s immune system attacking the pericardium.

Each immune system attack causes inflammation that leads to more immune system response in an ongoing cycle.
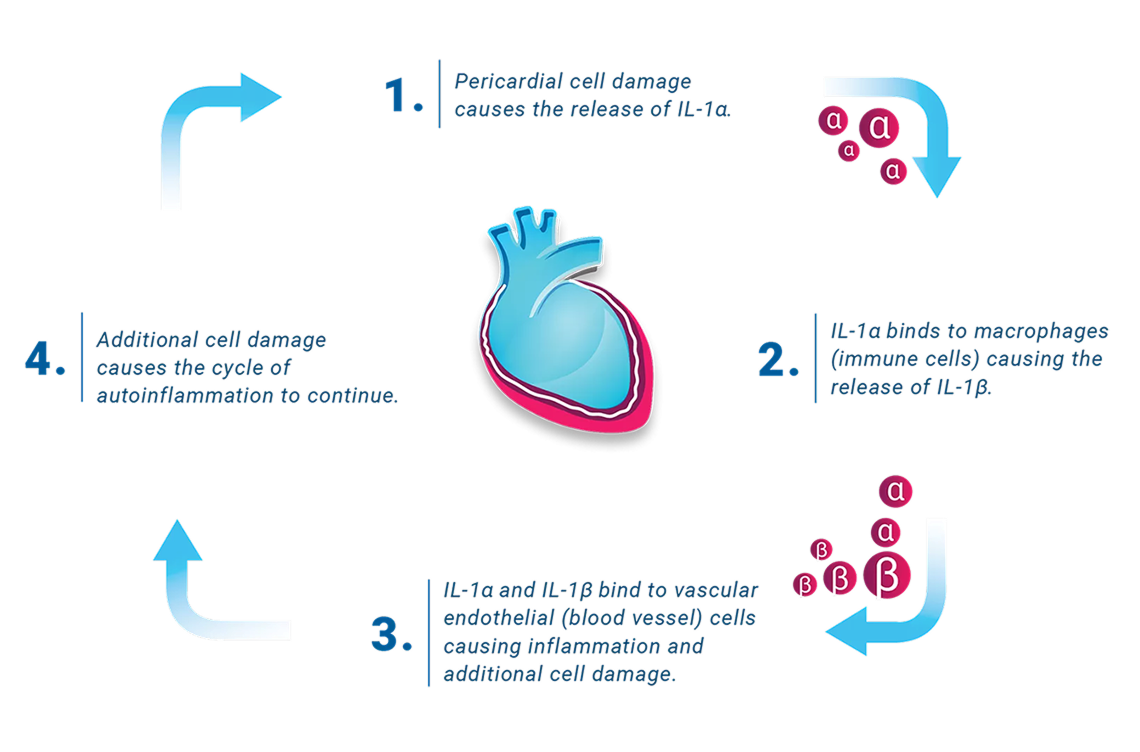
UNDERSTANDING THE CYCLE OF AUTOINFLAMMATION THAT DRIVES RECURRENT PERICARDITIS
Recurrent pericarditis occurs when proteins called IL-1α and IL-1β signal the immune system to attack the pericardium. Each attack causes inflammation that leads to more attacks in an ongoing cycle of autoinflammation.
Traditional oral therapies—such as nonsteroidal anti-inflammatory drugs (NSAIDs), colchicine, and corticosteroids—are often used to manage symptoms of a first episode of pericarditis. Treatment for recurrent pericarditis needs a different approach because traditional oral therapies do not specifically target the ongoing cycle of autoinflammation that causes recurrent pericarditis.
Long-term treatment of flares may require a treatment that can break the cycle of autoinflammation.
Managing recurrent pericarditis
If you have recurrent pericarditis, chances are that most of your care will be provided by a cardiologist (heart specialist).
Depending on your situation, you may also see:
This is not a complete list. The care you receive will depend on your medical history and the kind of care available to you.


THE IMPORTANCE OF BEING YOUR OWN BEST ADVOCATE
With a “rare disease” like recurrent pericarditis, it is especially important that you communicate with your doctor how the disease is affecting your life and what you need from treatment and from your care team.
These results from a poll of people with recurrent pericarditis showed that while the disease had a significant impact on their lives, both physically and emotionally, there is a need for better communication between doctors and their patients with recurrent pericarditis.
Impact of recurrent pericarditis
98%
feel that recurrent pericarditis disrupts their life in the time between flares.
90%
even after a experience negative physical, mental, or emotional impact from flares, even after a flare has resolved.
86%
worry they could have a flare at any time.
74%
have withdrawn from many aspects of life due to fear or anxiety about having a flare.
70%
missed important events or functions because of their recurrent pericarditis.
Quality of communication
Respondents said they had to go to an average of 3 doctors before being diagnosed.
88%
want their doctor to ask more questions about recurrent pericarditis and/or flares.
85%
often feel they "fall through the cracks."
90%
would like a treatment that prevents would like future flares better than their current treatment.
This survey was conducted online within the United States by The Harris Poll on behalf of Kiniksa Pharmaceuticals from May 4 to June 1, 2023, among 125 US adults ages 18+ who have been diagnosed with recurrent pericarditis and are not currently pregnant or breastfeeding and have never used/are not currently using an IL-1 antagonist. The sampling precision of Harris online polls is measured by using a Bayesian credible interval. For this study, the sample data are accurate to within +/- 8.7 percentage points using a 95% confidence level.

Tips from Yvette
A working mother of 2 active teenagers. Diagnosed with recurrent pericarditis in 2021.
Yvette suffered for over a year. Her journey included misdiagnosis, emergency room visits, inadequate treatment, and surgery on her heart. Based on her experience, here are a few tips for other people with recurrent pericarditis:
Advocate for yourself
Recurrent pericarditis is a rare disease. Many doctors may not recognize it or know how to treat it, so learn all you can, and when you talk to your doctor, don’t just listen. Make it an active conversation:
- Come with notes regarding your symptoms
- Research possible treatments and discuss them during your visit
- Write down any questions you may have, and write down or record your doctor’s answers
- Communicate your goals for treatment
Take care of your mental health
A therapist cannot diagnose or treat recurrent pericarditis, but if your disease is making you anxious or depressed, a mental health professional may be able to help.
Participate in a support group
Friends and family may be helpful and supportive, but it can also be invaluable to have people in your life who have shared similar experiences with recurrent pericarditis.
Treating recurrent pericarditis
After you have been diagnosed, your doctor will prescribe a treatment or treatments to help manage your recurrent pericarditis.
Medications used to help manage symptoms
Oral traditional therapies†—such as NSAIDs, colchicine, and corticosteroids—are often used to manage symptoms of a first or one-time episode of pericarditis.
- Doctors often try to limit the use of corticosteroids due to side effects and that steroids may contribute to recurrent pericarditis lasting longer
Treatment for recurrent pericarditis needs a different approach because these traditional therapies:
- Do not specifically target the ongoing cycle of autoinflammation that causes recurrent pericarditis
†Not FDA approved to treat recurrent pericarditis.

Medication indicated to treat recurrent pericarditis
- ARCALYST (rilonacept) is the first and only FDA-approved therapy to treat recurrent pericarditis and reduce the risk of future flares in people 12 years and older
- ARCALYST breaks the cycle of autoinflammation that causes recurrent pericarditis by blocking interleukin-1 (IL-1) signaling
If you experience another flare more than 4 weeks after one ends, ask your healthcare provider about ARCALYST.